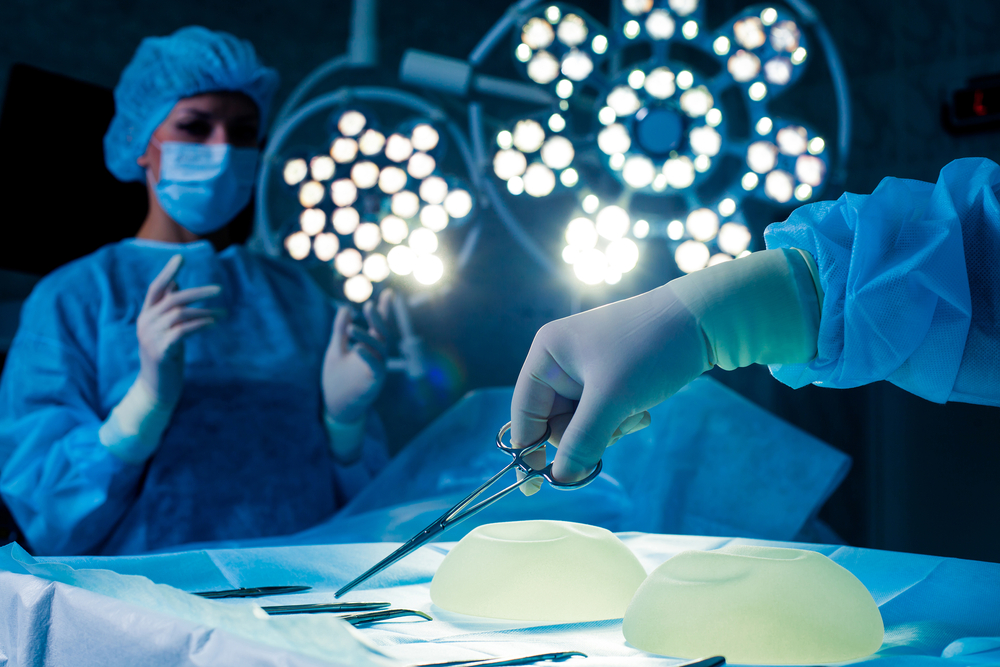
I want to address yet another plastic surgery “trend” aka hustle: 24-hour breast augmentation recovery. As expected, many synonyms have popped up like mushrooms to capitalize on this trend, including “flash recovery breast augmentation,” “rapid recovery breast augmentation,” “24-hour rapid recovery breast augmentation,” etc. etc. Breast augmentation is the second most common cosmetic procedure performed by plastic surgeons in the US. Around 300,000 procedures are performed annually. Not surprisingly, it’s a very competitive market and thus a lot of creative marketing language and pseudoscientific blather has been generated to gain an advantage in cyberspace.
Is 24-Hour Breast Augmentation Recovery A Real Thing?
The generic features of the 24-hour recovery breast augmentation are valid and align with the enhanced recovery principles I have used in my practice since 2015. They can improve care (and potentially outcomes), safety, pain levels, and the overall patient experience. However, the claims themselves are exaggerated in my opinion, and are not a derivative of what I would qualify as “science.” There have been no controlled trials. There is not a large body of studies with adequate statistical data to suggest clinical significance. In scientific jargon, the evidence is “anecdotal.” The grand poohbah or apostle of the 24-hour breast augmentation was John Tebbetts out of UT Southwestern. He published a two-part series, describing his approach (https://pubmed.ncbi.nlm.nih.gov/11786826/ and https://pubmed.ncbi.nlm.nih.gov/17099488/). Many of his disciples have actively promoted this approach, including Dr. Bill Adams (https://pubmed.ncbi.nlm.nih.gov/19050543/). Some of the salient features have been adopted in various forms by the plastic surgery community which are as follows:
- Delicate atraumatic surgical technique that relies on direct vision rather than blunt or blind dissection
- Through a specific sequence of steps, the actual muscle damage is minimized with release of the pectoralis major only is released. When additional muscle groups are damaged, such as the pectoralis minor and serratus anterior laterally, there is a LOT more pain. This is one reason why the total submuscular augmentation was abandoned in favor of partial muscle coverage due to prolong, recoveries and extreme pain.
- Minimizing blood in the cavity. Blood is inflammatory in nature and can lead to more pain, a slower recovery and potentially capsular contracture.
- A “no-touch” technique when it comes to the ribs. The ribs and periosteum are very sensitive and painful when injured so staying off them helps.
- Optimal use of muscle relaxants intraoperatively to make sure the muscle can be tented or retracted with minimal effort and trauma.
- Modified or improved instrumentation to improve the procedure and minimize trauma.
- Early mobility
Dr. Tebbetts’ principles and dedication to the surgical process was fairly profound (he was an engineer and extremely OCD) and bore good fruit. It’s not a miracle. It doesn’t guarantee ideal outcomes. It does improve pain levels and speed recovery. I believe many of these principles are simply an extension of enhance recovery approach which is sound.
Another point I want to emphasize here is proper size choice. Many patients experience increased pain and some of this is due to implants that are too large for their frame. I always talk to my patients about this before any decisions are made. I am a proponent of the subfascial approach, which does not violate any musculature whatsoever and has lower pain levels than even versus the Tebbetts 24-hour theology. You lose NONE of the pectoralis major muscle strength. Surgeons in Brazil and other parts of the globe favor this approach over the submuscular approach which is honestly a holdover in the plastic surgery community in the US from the 1980s. For patients with appropriate anatomy, this is my favorite approach!